UCPI - Our Services
Transurethral Microwave Therapy (TUMT) for Benign Prostatic Hyperplasia
What is benign prostatic hyperplasia (BPH)?
Benign prostatic hyperplasia (BPH) is nonmalignant (noncancerous) enlargement of the prostate gland, a common occurrence in older men. It is also known as benign prostatic hypertrophy and abbreviated as BPH. It leads to symptoms of urinary hesitancy, frequent urination, dysuria (painful urination), increased risk of urinary tract infections, and urinary retention. Although prostate specific antigen levels may be elevated in these patients because of increased organ volume and inflammation due to urinary tract infections.
Adenomatous prostatic growth is believed to begin at approximately age 30 years. An estimated 50% of men have histological evidence of BPH by age 50 years and 75% by age 80 years; in 40–50% of these men, BPH becomes clinically significant.
What are the symptoms?
BPH causes urinary problems such as:
Trouble getting a urine stream started and completely stopped (dribbling).
Often feeling like you need to urinate. This feeling may even wake you up at night.
A weak urine stream.
A sense that your bladder is not completely empty after you urinate.
In a small number of cases, BPH may cause the bladder to be blocked, making it impossible or extremely hard to urinate. This problem may cause backed-up urine (urinary retention), leading to bladder infections or stones or kidney damage.
BPH does not cause prostate cancer and does not affect a man's ability to father children. It does not cause erection problems.
What treatments are available?
Thermotherapy, the newest treatment option for BPH, is a non-surgical, outpatient alternative that improves symptoms and urine flow with no serious side effects. UCPI offers transurethral microwave therapy, a safe and effective method used in the treatment of lower urinary tract.
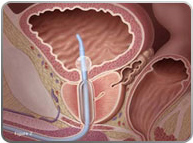
In transurethral microwave therapy (TUMT), an instrument (called an antenna) that sends out microwave energy is inserted through the urethra to a location inside the prostate. Microwave energy is then used to heat the inside of the prostate. Cooling fluid is circulated around the microwave antenna to prevent heat from damaging the wall of the urethra. To prevent the temperature from getting too high outside the prostate, a temperature sensor is inserted into the man's rectum during the procedure. If the temperature in the rectum increases too much, the treatment is turned off automatically until the temperature goes back down.
The temperature becomes high enough inside the prostate to kill some of the tissue. As this part of the prostate heals, it shrinks, reducing the blockage of urine flow. This treatment is done in a single session. It usually does not require an overnight stay in the hospital. A general or spinal anesthetic is needed during the procedure.

What To Expect After the Procedure
You are generally able to go home after the procedure. You may not be able to urinate and may require catheterization to drain your bladder. For most men, this lasts for a week or less. You may also have to take antibiotics or anti-inflammatory medicines. You can generally return to work 1 to 2 days after treatment. Sexual activity can be resumed 1 to 2 weeks after surgery. (2)
Efficacy of TUMT
In conclusion, TUMT is a safe and effective, minimally invasive, alternative treatment for symptomatic BPH. TUMT can be performed in a 1- to 2-hour office visit, without intravenous sedation. The procedure therefore is an alternative for patients who are at high surgical and anesthetic risk. It is not effective for patients with a large median lobe or a very large prostate, and it results in less-significant improvement in urinary flow patterns than does TURP.
TUMT appears to balance efficacy against patient tolerability, although this balance might be tenuous for patients long-term.
Fitzpatrick JM (2007). Minimally invasive and endoscopic management of benign prostatic hyperplasia. In AJ Wein, ed., Campbell-Walsh Urology, 9th ed., vol. 3. pp. 2803-2844. Philadelphia: Saunders Elsevier.
Webber R (2006). Benign prostatic hyperplasia, search date May 2005. Online version of BMJ Clinical Evidence. Also available online: http://www.clinicalevidence.com.
Rubenstein, Jonathan; McVary, Kevin T. (6 February 2008), "Transurethral Microwave Thermotherapy of the Prostate (TUMT)". eMedicine.
WILLIAM C. SHIEL JR., MD, FACP, FACR, CHIEF EDITOR. chief editor for MedicineNet.com since he co-founded it in 1996.
1995-2011 Healthwise, Incorporated. Healthwise, Healthwise for every health decision, and the Healthwise logo are trademarks of Healthwise, Incorporated.